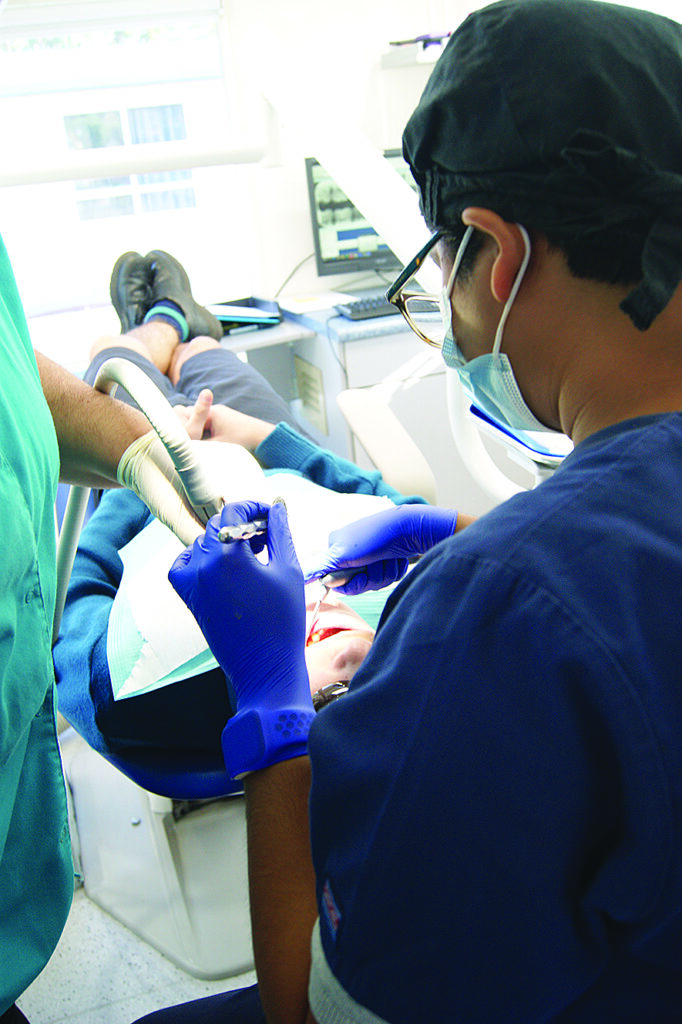
A children’s health report (TV1 News, 22 June 2022) uncovered alarming rates of poor dental health for 40 per cent of our country’s five-year-olds. The research was undertaken by ‘Cure Kids’, New Zealand’s largest charitable funder of medical and scientific research for children’s health. The report testifies that, ‘ . . . it partnered with the Paediatric Society of New Zealand, the Royal Australasian College of Physicians, and the New Zealand Child and Youth Epidemiology Service at the University of Otago, to analyse data for the report.’
The TV1 news report read, ‘Data from 2019 revealed that 41% of five-year-olds had evidence of tooth decay, that rates of tooth decay and hospitalisation were consistently the highest for Māori and Pacific Island children, and those living in the most deprived areas had three times the number of tooth extractions as those in the least deprived areas.’
The report also found rates of hospitalisations for children with serious dental decay had increased steadily since 2000, despite average rates of decay declining overall.
The research also examined other health markers in children and prompted the Children’s Commissioner, Frances Eivers, to say, ‘On many measures, New Zealand is currently one of the worst places in the developed world to be a child.’
Harsh words indeed from our Children’s Commissioner. It is not that we don’t know child poverty exists, it is alarming that it has become so pervasive. Societal inequities are now feasting on a generation’s future.
Whilst poverty undoubtedly influences the dental health of our young ones, there is another factor one might loosely call, a ‘hangover from the past’ that deters families from seeking dental care. The Listener, 3 July, 2021, captured the history of New Zealand’s publicly funded school dental service well. The article was entitled ‘Tales of the Murder house’, a chilling encapsulation. The article reveals that in New Zealand, the school dental service began 100 years ago. We were the first country in the word to establish free school dental care. All medium to large schools boasted a dental clinic, staffed by a fully qualified dental nurse. If your school was too small to have a clinic, you were ushered off to a nearby school that did. Every child received an annual check up and short of orthodontic specialist procedures, for which you were sent to a dentist, the dental nurse took care of children’s oral health needs. From my own personal experience, the nurse would also give you unequivocal instructions on how to brush your teeth and sometimes your visit might include a spontaneous ‘lecture in nutrition’ to dissuade you from eating sweets.
So why the ‘Murder House’? In part, dental clinics earned this label from the outdated tools that equipped the clinics and the tendency of nurses to ‘drill and fill’, as the Listener article explained. Children had to endure the slow, belt-driven, ‘pedal power’ treadle drills operated by our dental nurses even though by 1949, a Kiwi dentist had invented the high-speed drill. They also had very low dosage and largely ineffective anaesthetic for tooth extractions and nurses were not allowed to use the nerve blockscommonly used by dental nurses in Australia, Canada and other countries. It was argued that the risks of new equipment like the high-speed drill and nerve blockers were too high for our dental nurses who were not trained in their use.
Nurses in turn were instructed to fill even the tiniest of cavities with the silver and mercury filling compound, later found to be a potent neurotoxin. The logic behind this practice was to prevent future decay and extractions but is now seen as somewhat misguided reasoning.
Reports from youngsters of the time show that the expectation of a visit to the dental nurse was associated with high anxiety and dread. Whether every child’s dental visit was a highly painful experience is doubtful, but this fear and loathing of the dental clinic became embedded in the psyche of several generations of Kiwi kids. Despite the horror stories, the school dental nurses performed an important function, keeping check on the dental health of our nation’s children. There’s something to be said for a dental service that was free, compulsory, and regular.
School Dental Clinics were phased out in the 1990s, mainly because the buildings had not been maintained and the costs of upgrading equipment was prohibitive. Instead, the Government would fund dental care, through contracts with local District Health Boards (DHBs), for children up to secondary school age, and later up to age eighteen. Children and young people would attend their own family dentist for free treatment.
We may well ask, if dental care for our young people is free up to age 18, why are they not regularly attending their dentist? The answer is multi-faceted. For many youngsters, it is not easy to access the dentist without a parent taking a day off work to get them there. For others, dental health is not top of mind given the complexities of some families, especially those living in poverty or who are low paid shift workers or the working poor. We now see the results of the shift from attending the dental clinic at school to attending your own private dentist in town. It means 40 per cent of five-year-olds suffer tooth decay and it is worse if you are Māori or a Pacific Islander.
One excellent answer to this dilemma is to have mobile dental units setting up on school grounds, only this time, the dental units would have state of the art equipment. That is the concept Dental Planet has adopted. Alfred Rico, general manager of Dental Planet took me to visit two of their mobile units. One was operating out of Glendowie College carpark in Auckland’s Eastern suburbs and the other was on the school grounds of a Glen Eden Kura Kaupapa Māori School in South Auckland. I spoke to some of the students attending the service.
Rogan, at Glendowie College, told me that year 13 students, such as himself, have their dental treatment in the first term of school, ‘ . . . so that the dental visit doesn’t interfere with assessments.’ He was pleased to attend the mobile unit because it meant his teeth were checked and x-rayed every year and it was all painless enough. More importantly, it all occurred at school and didn’t disrupt his learning.
Another Glendowie student, waiting for his check-up, told me a similar story. He probably wouldn’t be getting his teeth checked if he had to go to his own dentist, because of the time to get there and back. He was enrolled with the mobile dental unit because it was right here on the school grounds, and he could have his check up during school hours.
The key to the popularity of the Glendowie College mobile dental clinic was the connection with the school. Through the relationships built up with the school Dental Planet has a good understanding of the students’ schedules, the school understands what Dental Planet is trying to achieve for the students’ dental health, and they work together in partnership.
In the South Auckland Kura, the two dental chairs in the mobile unit were both occupied, and more students were waiting their turn. The Oral Health Therapists (OHTs) working on the students’ teeth engaged easily with the students, some of whom were concerned about how they would continue with their dental health once they were out of school and over 18 years old.
‘It is so important to have these students’ teeth in the very best condition possible,’ said Patrick, one of the Dental Assistants, ‘because once they have left school, they might not see a dentist again for a very long time.’
Patrick, of Pacific Island descent, joined the mobile unit team straight out of school. He has been trained by Dental Planet to be a Dental Assistant which includes a yearlong course. Dental Planet paid his fees. He would now love to continue to train as an OHT, and perhaps even win a scholarship to train as a dentist one day. ‘I love this work,’ he says, ‘and just want to go on, learn more and one day become a dentist,’ he said. ‘Dental Planet has given me the start to a great job, and I want to keep going.’
Alfred explained that through their careers programme, they want to encourage especially Māori and Pacific Island secondary students to make dentistry their chosen profession. To achieve this goal, they work alongside careers advisors in schools and the ‘Gateway’ programme, which provides students with structured workplace learning across a range of industries while they continue to study at school. By giving interested students a taste of dentistry, they have managed to attract those like Patrick, to train with them.
Whilst they currently offer five full scholarships a year for OHT training and Hygienist training, they want to build on that. They want to offer many more scholarships and include support for a full dentistry degree for some of those who aspire to be fully qualified dentists.
The Dental Planet team’s interest in improving dental health is not limited to the students, they also offer free annual hygienist appointments for the school staff and 10 per cent discount on any dentistry work a staff member requires. Further, they encourage the students to bring their parents to the local Dental Planet Surgeries, where they will be assisted in accessing any dental health subsidy they are entitled to.
The mobile service so far reaches only secondary schools, although Alfred assures me the company is very keen to extend their services to primary and middle schools as well. They are a new company and so far, operate mobile clinics and dental surgeries in Auckland and mobile units in the Waikato. They are aware of the inequities in dental care and that is why they have chosen to set up mobile units initially in South Auckland. They also work alongside Māori Health providers to encourage whānau to ‘take the chair’ and have their teeth checked too. In some cases, the Māori Health providers cover the costs of dental care for their people so that there is no financial barrier to accessing the oral treatment they need.
‘We have our own surgeries in South Auckland but not yet in the Waikato. For now, staff of Waikato schools are treated in the mobile units, just like the students,’ explained Rico.
Education is just as important as dental treatment for the Dental Planet team. ‘We ask schools to give us some of their assembly time to educate students in how to take care of their own teeth better,’ says Alfred. ‘This is part of our programme to prevent teeth developing decay in the first place,’ he said.
Thinking to the future, the Dental Planet team is already looking to acquire further agreements with the Auckland, Waitemata and Counties Manukau DHBs to help primary and intermediate aged students, and to expand services in the Waikato region. The team also recognise that adults could benefit from having mobile dental units in their communities. ‘Not all people have access to our dental surgeries or any other dental surgeries,’ says Rico. ‘That is where our mobile units are so useful because we can take our services to the people.’
The Dental Planet team may not yet be the complete alternative to the free, compulsory, regular dental service every school aged child once had in Aotearoa New Zealand, but they are a responsive, modern, mobile dental health service, meeting the needs of many thousands of young people today, at least in the South Auckland and Waikato regions.